In a rather shocking news released by researchers, the United States of America has been witnessing a significant rise in the number of colorectal and gastrointestinal cancers, under the age of 50 especially.
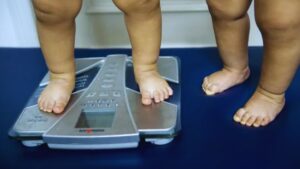
An increased risk of early onset of gastrointestinal cancers is associated with obesity, which is also rising in the U.S at a rampant rate. That’s what scientists say is a leading theory for the surge – with a 2019 study proving that women who were considered obese had nearly double the risk of developing colorectal cancer. Close to half of all U.S. adults are predicted to be obese by 2030, according to research released the same year.
The chronic condition can cause inflammation and higher levels of insulin that increases peoples’ risk of getting cancer, including several types of gastrointestinal cancers, a deeply disturbing thought for the educated adult of today. In the United States, several other risk factors including smoking, drinking alcohol, eating a heavy diet can also play a major part in the cancer built up.
Earlier this year in 2025, new research pointed to the impact of a toxin in the gut, known as colibactin, that can inflict DNA damage on colon cells, and could potentially lead to the development of cancer. Colibactin is produced by the bacteria E. Coli, which is often responsible for foodborne related illness in human body. As of now, the specific cause remains unclear, but the U.S. is not alone, researchers said. The incidence of GI cancers in adults younger than age 50 is rising globally actually, an alarming sign that must be addressed and looked into on priority.
But specifically in the U.S., the early onset-cases have shown a consistent increase, in both American men and women since the mid-1990s. In comparison to American adults born in 1950, those born in 1990 have twice the risk of developing colon cancer and four times the risk of developing rectal cancer, the researchers found. The influence of a diet is paramount in deciding such outcomes ahead.
The unexpected early arrival colon cancer has become the leading cause of majority of the cancer-related deaths in U.S. for men under 50. For women in the same age group, it’s the second-leading cause of cancer-related deaths. The colorectal cancer is also known to have fatal impacts on Hispanic, Indigenous and Asian communities too, but rather disproportionately.
Way Ahead
These findings signal a worrying shift and potentially indicate the need for updated treatment practices. Patients with early-onset colon cancers often experience delays in diagnosis because neither doctors, nor the victim’s suspect cancer as an existing condition; with a more accurate diagnosis occurring only when the patients at advanced stages of the disease.
Overall, colorectal cancer has emerged as the second most common cause of U.S. cancer deaths, and as per the American Cancer Society, the count is expected to cause about 52,900 deaths this year, which is disturbing.
The need of the hour is to develop more effective screening, prevention, and treatment strategies to detect the and investigate the biology of early-onset GI cancers, so that necessary actions can be undertaken. In addition, the fat-coated and rather heavy American diet must see a shift, in order to control the figure. The US FDA in association with the American Cancer Institute, spearheaded by Trump’s health ministry must brainstorm to develop some stringent prevention measures to reduce the rise of cases.
Helene Elliott is the senior reporter for News Raise. She covers Science news. She also has a keen interest in photojournalism. Helene holds a nomination for the prestigious Red Smith Award. She is married to author Dennis D’Agostino, a former publicist with the New York Mets.